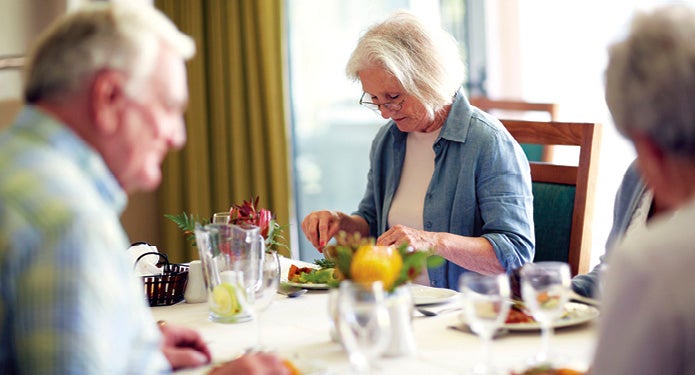You can use a person-centered approach to everyday eating that builds connections and provides nutrition
Throughout life, connections with friends and family help people lead content and satisfying lives. “That doesn’t go away when a person has Alzheimer’s,” says Ruth Drew, director of family and information services for Alzheimer’s Association, a Chicago-based national nonprofit dedicated to researching the disease and caring for and supporting those affected by Alzheimer’s.
Normal, everyday activities like mealtimes help people with Alzheimer’s and those with other types of dementia connect with others, maintain a good quality of life and sustain their sense of self.
A routine around mealtimes for residents in memory care units can go a long way toward caring for this vulnerable population, while helping them maintain existing connections and encourage new ones. And it all starts by focusing on each individual resident.
“More and more, I am seeing a person-centred approach,” Drew says. That person-by-person solution, versus a one-size-fits-all method, ensures pleasant and productive mealtimes for all residents, even as three rules hold sway: residents should be empowered to eat with dignity, the food must be nutritious and good-tasting, and both the dining environment and way the food is served needs to encourage eating.
3 ways to promote dignity and cut confusion
1. Use the power of choice. This maintains a patient’s dignity, provides a home-like atmosphere and gives residents more control over their lives. But Drew advises limiting their selections to two options instead of five, so they don’t get overwhelmed. If they appear confused, staff can step in and help them make a decision.
2. Serve foods one at a time. Offer fruit first, then eggs, then toast, for instance. Serving on coloured plates also helps, because it makes the food stand out. For residents with tremors or a tendancy to wander, finger foods are ideal—say an egg sandwich, rather than eggs and toast.
3. Maintain a routine. Serve meals in the same place, at the same time, with the same people. “Their brains struggle with processing new things,” Drew says. That same place should also be quiet, as noise can overstimulate patients and produce anxiety. A smaller table, say four people, in a carpeted area, creates the right atmosphere.
Improve the residents’ experience
“We are caring for people at a state of life where the majority of them would prefer not to be there,” says Neil Prashad, president and CEO of Origin Active Lifestyle Communities, a collection of retirement communities in British Columbia and Alberta, Canada. “We all understand the circle of life, we understand we need that assistance, but the bottom line is [finding] a way to make that experience as normalized and enhanced as possible,” he says.
At Origin, “enhanced” means improving the experience of dining in the same place, with the same people, three times a day. “Normalized” means making dining as adult-like as possible. “If you focus on normalization, food shouldn’t come out of a hole in the wall already plated and chosen,” Prashad says.
To make dining in memory-care units more normal and less institutional, Origin has rethought pretty much everything. Dining with disposable or plastic dinnerware isn’t normal, nor is fancy china at every meal. “We want the same mismatched stuff you have at home,” Prashad says.
“Normal” means family-style service, as most residents didn’t grow up with restaurant-style table service for 21 meals a week. “We put a pile of toast in the middle of the table,” Prashad says, adding that caregivers plate food and serve it to residents who are not able to help themselves.
It also means asking residents who are able and willing to set the table, fold napkins, and otherwise help prepare for the meal. After the table is set, residents sit down to enjoy the meal and converse with others at their table, similar to how they would have sat down and chatted with relatives in their own dining room.
Use aroma to draw diners
The food is prepared in open kitchens that allow the scent of what’s cooking to waft into the dining areas. Aroma works wonders in stimulating appetites, which is one reason why Origin kitchens frequently bake bread and other fragrant foods. This strategy, Prashad says, has lured frail residents out of bed for mealtime. “They talk about the fact that their appetite really isn’t there, but they come [to the dining room] anyway,” he says.
As for meal components, “there’s no magic to it,” Prashad says. Even though labour costs are higher, Origin kitchens make as much food from scratch, using as many top-quality ingredients as possible. For mashed potatoes, for instance, the staff peels and boils real potatoes. Each kitchen also has a hydroponic herb garden, which enables chefs to add fresh and natural flavours to dishes.
Your Gordon Food Service Sales Representative can provide recipes and ideas to stimulate appetites, as well as specialized tableware to meet the needs and abilities of memory-care residents and patients.
In addition to a “normal” and “enhanced” dining experience, flexibility is important with memory-care patients. Cognition levels can change, even day to day, so staff are enouraged to flex as the cognition levels of their residents dictate. “It’s a work in progress,” Prashad says.
Like any good work in progress, Origin will continue to “normalize” and “enhance” life for its memory-care patients and residents, and Prashad is rather looking forward to what the future holds. “This is such an awesome business to be in if you are open to change and innovation,” he adds.
Helpful Resources
There are places healthcare professionals can go to find ways to better serve people with Alzheimer’s and dementia:
1. The Alzheimer’s Association, a Chicago-based nonprofit, has a booklet: Dementia Care Practice Recommendations for Assisted Living Residences and Nursing Homes.
2. A 24/7 help line for healthcare professionals, families and caregivers. That number is 1-800-272-3900.
3. Alzheimer Society Canada message board for healthcare professionals. Their 1-800-616-8816.